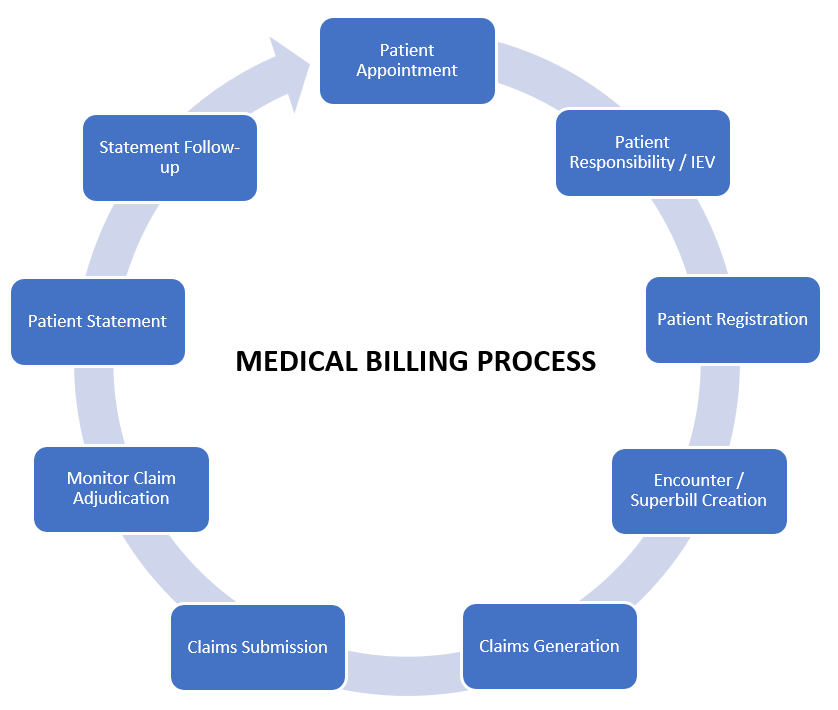
The medical billing process can be equally complex and frustrating for providers and patients. To get paid, providers must submit accurate and complete claims to insurance companies, which can be time-consuming.
What’s more, insurance companies often deny claims or only pay a portion of the billed amount, which can lead to significant reductions in revenue. As a result, improving medical billing and collections is a top priority for many healthcare organizations.
In this article, we will provide five medical billing tips to improve collections. By following these tips, you can decrease claim denial rates, improve cash flow, and increase your overall revenue.
- Provide your front-office staff with the appropriate training to explain patient responsibilities to them upfront.
Front office staff must be prepared to have difficult patient conversations about co-pays, deductibles, and other patient responsibilities. Many companies today utilize advanced technological solutions to make medical billing easier. To explain the benefits to the patient in a practical way, the staff should be aware of notable features such as claim audit trails/claim histories, seamless Claim Status Enquiries (CSI), online payments, etc., that these solutions provide. This way, they can explain to the patient effectively the amount that one must pay, be able to collect the required dollars, and manage the revenue effectively. However, if the patient senses uncertainty from the staff, they will be less likely to pay the money.
- Be transparent with the pricing.
Consumers often have difficulty comparing prices among providers because they don’t know what services are included in the price. Providers can help bridge this gap by informing the patient before their visit or letting them know when they come in for the appointment. There are times when they may have to pay for secondary insurance in addition to their primary policy. In certain situations, they may also have to owe secondary insurance along with their primary plan. The more they are aware of all these factors, the more likely they will be to pay the amount rather than mounting the bills.
- Move the revenue cycle to the front office rather than the back office.
Every employer must ensure to provide their staff with comprehensive training so that the employees understand not only their work, but also the work of their colleagues. In addition, it might also be prudent that the front office employees be familiar with which policies can pay on claims or which do not. By having access to information like this, they will be able to educate the patient in depth about why they must pay a certain amount.
- Provide consumer-friendly electronic payment options.
With telemedicine taking the forefront of the industry, it is vital for healthcare clinics also to provide payment options that work with patients’ digital lifestyles. For example, you can accept major credit cards, offer automated bill payment services, or even promote the use of online wallets such as expEDIum Pay® or similar ones. By offering electronic payments, providers make it easier for patients to make their payments on time. In turn, this can help to reduce the chance of patients missing payments and incurring fees, which can lead to claim denials.
- Utilize technological payment solutions to your advantage.
Healthcare Financial Management Association reports that while employers claim their solutions are reliable, outdated interfaces, limited interoperability between systems, and inadequate data management capacity are common issues. Therefore, finding solutions to these and other frustrations can help organizations use automated solutions more effectively. Usually, clinics handle all payment-related matters themselves or outsource them to reputed medical billing companies.
With our expEDIum Medical Billing Software, you will find that it provides end-to-end software management solutions for clinics and outsource their billing operations. We utilize our partners to take care of eligibility verification, clearinghouse solutions, billing, and other services. Many companies also routinely send billing information by secure emails, and perhaps that is something you could consider implementing.
Conclusion
When running a successful business, efficient billing and collection processes are essential for a medical practice. Unfortunately, with the increasing number of insurance companies building documentation requirements into their contracts, many medical professionals are dealing with an ever-increasing number of difficult patients. It’s impossible for any doctor or clinic to process all their documents in less than two days.
One key aspect of your practice’s success is ensuring that every individual patient pays their portion of the bill. By implementing these five tips into your operation, you’re sure to increase your cash flow and ensure that all incoming payments are being collected effectively. If you need help with medical billing and collections, contact iTech Workshop or explore the features of our product expEDIum here.